Jaundice is a frustrating subject. Every time I hear a result, each time a family shares with me their concern about the number they heard, I wonder what we are measuring, why we are doing it, what we are trying to prevent and for all the work we are doing, what meaningful outcomes we are actually seeing. I also wonder if we are doing any harm.
Most hospitals, if they are following the American Academy of Pediatrics (AAP) guidelines, are screening every baby and assessing their jaundice risk prior to discharge. A screening test, especially one done on every child, ought to be pretty good and really necessary. That is a hard sell for me.
Definitions
First, before I go any further, we need some definitions. Jaundice is the term we use to describe the yellow discoloration of the skin that comes from elevated levels of bilirubin. Bilirubin is a yellow product of the breakdown of red blood cells, specifically the breakdown of the heme component of the red blood cell. High levels of bilirubin are called “hyperbilirubinemia.” (We can dissect that word: hyper=high; emia= in the blood. Therefore, hyperbilirubinemia is high bilirubin in the blood.)
So “jaundice” is not really a disease- it is a color. Hyperbilirubinemia is a description of high levels of bilirubin, and bilirubin comes from a breakdown of red bloods cells. Hyperbilirubinemia usually means liver disease, but by itself, remains a description. In the immediate newborn period, the great majority of healthy, term newborns will have hyperbilirubinemia, with levels peaking somewhere around days 4-6 of life, and gradually decreasing from there.
I am clarifying this because historically high levels of bilirubin have been considered a disease in the healthy, term newborn. But what if high levels of bilirubin are normal and helpful to most healthy, term newborns? If most babies “have jaundice” (which you now know means “have yellow coloring”) maybe those levels of bilirubin are supposed to be high.
Bilirubin as a disease in newborns: the history of the worry
Bilirubin can be a toxin, crossing the blood-brain barrier and causing brain injury. The blood-brain barrier is very protective, maintaining a huge wall between the bloodstream and the cerebral spinal fluid. When all is working well, nothing can cross that barrier without an invitation. In newborns, however, that barrier is leaky. (I feel as if every time I wrote about something related to breastfeeding, I am writing about something leaky!) The leaky newborn blood-brain barrier can let bilirubin through, and at some level that we have not discovered, can cause injury. That injury is called bilirubin encephalopathy or kernicterus. Kernicterus is awful, permanent, devastating and completely preventable with current therapies. (On a potentially powerful side note, “completely preventable” means if it occurs, in addition to the horrors of the injury, it is also a likely lawsuit.)
Medicine was introduced to kernicterus in the early 1900s, when researchers noticed yellow discoloration of the basal ganglia (a part of the brain) during autopsies of babies who most likely had a problem called Rh Isoimmunization. The need to urgently identify and treat Rh Isoimmunization peaked in the 1950s-1970s. The Rh factor is a protein on the surface of a red blood cell. Most people have the protein, so they are Rh positive (Rh+). Those that don’t are Rh negative (Rh-). In Rh isoimmunization, an Rh- mother has a baby who is Rh+ and she makes antibodies against that Rh protein. That first baby is just fine, but mom keeps those antibodies against the Rh factor protein. The problem comes with the next baby. If that baby is Rh+, those antibodies mom made against the Rh protein start attacking the new baby’s Rh+ red blood cells. We know that bilirubin is created when red blood cells are destroyed. Because the baby’s red cells are being attacked, lots of bilirubin is produced. And bilirubin can cross the blood brain barrier. The researchers noted that a bilirubin level of about 20 mg/dl was the threshold for the yellow coloring in the brain to appear. When the medication Rhogam was invented, Rh isoimmunization was essentially wiped out and we started to relax a little about hyperbilirubinemia in newborns. But, from then on, bilirubin became a toxin and 20 became a dangerous number.
In the 1980s, researchers noted that breastfed babies were more likely to become jaundiced and the search started for the jaundice-causing mystery ingredient in breastmilk; because, bilirubin is a toxin, remember? What they did not know, or maybe they did, is that breastfeeding is normal, and what happens in breastfed kids is normal and physiologic. Maybe jaundice in healthy, term infants is actually normal. Maybe bilirubin is not always a toxin. But in the 1980s, we are just coming off of years where breastfeeding was hardly the cultural norm, so maybe it was too soon for that kind of thinking.
In 2004, the AAP suggests that all babies should be assessed before discharge for the risk of severe hyperbilirubinemia. In that statement, “exclusive breastfeeding, especially if not nursing well and excessive weight loss” is a major risk factor for hyperbilirubinemia. I find it hard to get my head around physiology being a risk factor. I get the “not nursing well” and you know my take on “excessive weight loss” but exclusive breastfeeding is normal. Maybe hyperbilirubinemia is normal. The timing was still probably premature for this type of thinking.
This same statement also gives us an algorithm for checking bilirubin and the nomogram onto which we plot the bilirubin. I’ll give you a few minutes to find the part where it says “assess breastfeeding.” Nah, don’t bother. It’s not there. (Hence, the inclusion of this algorithm in a nearly unreadable form.)
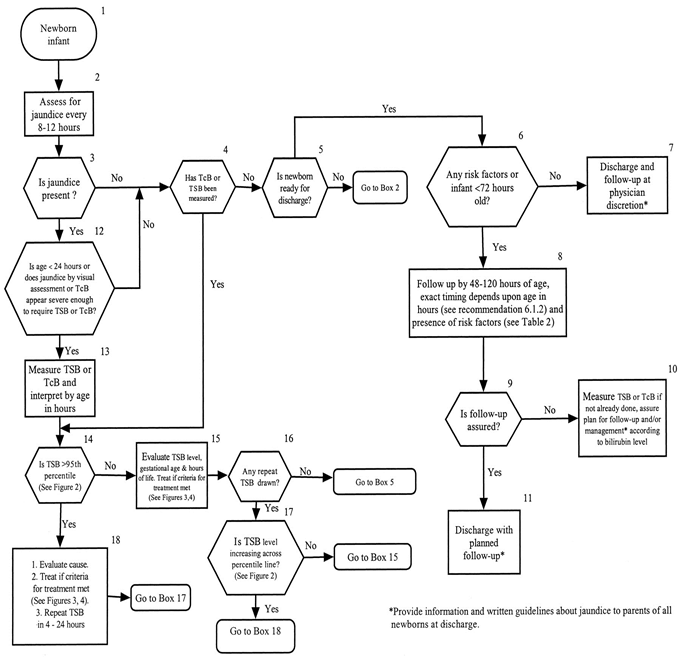
So, now we have something to measure, total serum bilirubin (TSB) and know what to do with that number. But the nomogram on which we are supposed to plot the baby’s TSB and make any future management decisions was created based on a sample where less than 60% of the babies were breastfed. So, the nomogram is not based on normal. Maybe it was still too early to question if we were doing the right thing.
In 2009, a commentary by experts in the field of neonatal jaundice suggested that all babies should have their bilirubin checked, regardless of risk factors, at the time of discharge and when any signs of jaundice appear. Then we plot that measured bilirubin on our nomogram and proceed with appropriate therapy. Interestingly, they admit that kernicterus can occur without elevated bilirubin, and that they do not know the incidence of kernicterus in the US. They also say that they do not know if their suggested interventions are cost-effective or if they even prevent kernicterus. Now I am confused. Really confused. We do not know what causes kernicterus, if we are doing the right thing, or if it is even helpful…but check every baby anyway.
But, you may say, it is really a simple thing to do, what’s the harm? Well, as mothers, we remember that number. This study, done in 1989 when we were still using risk factors to screen babies, says just by checking the total serum bilirubin, just by checking, an otherwise healthy infant, with or without treatment, can lead to adverse psychological and behavioral consequences. Mothers of babies who were checked were less likely to leave their child with anyone, more likely to seek medical attention, and more likely to stop breastfeeding. There is your harm.
Bilirubin as an antioxidant: an alternative theory where
bilirubin is not bad
Normally, a baby adapts to the low oxygen concentration of the womb (the babies are breathing through the placenta- not perfect) by creating more red blood cells. At birth, the baby does not need as many of those red blood cells and the extras are destroyed. As we have talked about, the inside of the red blood cell contains the yellow pigment, bilirubin. Therefore normal babies will have higher levels of bilirubin because normal newborn mechanisms produce those higher levels.
The normal, healthy term newborn gets rid of bilirubin when the liver changes it into a water-soluble form which can be then transported into bile. Once water-soluble bilirubin gets into the small intestine, many things can happen to it, like sneaking back into the bloodstream through a process called enterohepatic circulation. We could talk more about bilirubin metabolism, but I have decided to skip it, since I imagine that it would be pretty boring. (I actually know it is boring.) But in the end, the bilirubin comes out in the stool. And what helps stooling? Efficient transfer of breastmilk into that newborn gut.
That means, if we notice jaundice, we need to know how breastfeeding is going. One of the most common ingredients in breastmilk are oligosaccharides. They are non-digestible sugars that help develop the infant’s immune system by preventing inflammation. Because they are non-digestible, they come out in stool. Therefore, the more breastmilk the baby gets, the more oligosaccharides the baby gets, the more poop we get. The more poop we have, the more bilirubin that is excreted, and the less we need to worry about that jaundice we noticed. When we assess a healthy, term newborn, we need to know about poop. Effective breastfeeding causes greater stool output. Less effective breastfeeding causes less stool output. Fixing ineffective breastfeeding is one way we can help with bilirubin excretion. We need to work on "look at the baby" before we intervene with something other than human milk.
Then let’s look at the normal pattern of jaundice: should not normally be present in the first 24 hours, peaks at days 4-6 and then drops off with time, sometimes several weeks. Many species do not make bilirubin. They stop at the creation of biliverdin, another pigment produced by the breakdown of red blood cells, except this one is green and is easily excreted. Humans continue to the production of bilirubin, but the conversion of biliverdin to bilirubin takes energy, and anything that takes energy in a newborn should serve some great purpose. Hopefully, when we convert green to yellow, it serves a purpose.
You know that it would serve some great purpose, right? Biliverdin (green) is converted to bilirubin (yellow) by an enzyme (biliverdin reductase) in a reaction that requires energy. I have written before about the importance of avoiding inflammation in the newborn gut, so it should come as no surprise that bilirubin and biliverdin have a role in protecting the newborn from inflammation. Biliverdin has anti-inflammatory properties and bilirubin is an anti-oxidant like vitamin E. Even the enzyme that converts green to yellow has a role; bilverdin reductase is another regulator of the immune system response to inflammation.
Having a good supply of anti-inflammatory agents and anti-oxidants around makes sense. The conversion of biliverdin to bilirubin, and the resulting increase in bilirubin production in most healthy, term newborns is more likely an expected and valued part of the transition to being born than a really dangerous brain toxin. The process of creating extra bilirubin serves as an elegant anti-oxidant, anti-inflammatory bridge from the womb to the outside world, and does not waste the product of the normal breakdown of unneeded red blood cells. Cool system.
Having increased bilirubin, and therefore jaundice, is a smart way to transition a newborn to living life outside the womb. But some children have been injured from too much bilirubin. How did that happen?
The concept of free bilirubin
When we check the bilirubin level on a baby we are using a total serum bilirubin (TSB) which is the total bilirubin the bloodstream, or a transcutaneous bilirubin meter, where we put a little probe thingy on the baby’s forehead and get a measurement from the skin. Both of these measurements give us worthless information.
That may be a little harsh, but well, it is true. Total serum
bilirubin has
consistently been shown to be a poor risk indicator for kernicterus (I
linked to it, but since the study is a good one and well worth the read: here it
is again
http://pediatrics.aappublications.org/content/117/2/474.short. Make sure to
check out Figure 1: “Outcome
of newborns who were readmitted with severe hyperbilirubinemia, illustrating the
low specificity of TSB in predicting bilirubin neurotoxicity” because it is a
very powerful illustration of how much we are relying on a test that does not
work very well.)
What makes more sense is the concept of free bilirubin. Lots of things in the body, like thyroid hormone or testosterone, exist either bound and stuck in the blood stream without any effectiveness, or free and biologically active. It is the free part that does the work. Studies now show that bilirubin exists in a free and bound state and the free part is the one that sneaks across the blood-brain barrier and does the damage. So we really should be measuring free bilirubin levels if we are worried. But we can’t. No good tests have been developed yet.
If we are worried about free bilirubin, which I think we ought to be, then we need to be aware of which states create a situation where the bilirubin breaks from its binding like sepsis, acidosis, and hypoxia. Infants with those conditions are usually very sick, and ones who might not be breastfeeding well. We also need to worry about conditions where there is too much bilirubin to bind because too much is being made. The most important of those conditions is called hemolysis and it happens, frequently but not always, when mom and baby have different blood types.
The United States Preventive Services Task Force: not enough information to recommend all this screening
In order to have a good screening test, it should be able to
correctly predict that
a patient with
a positive test result has the disease (sensitivity) and that a patient with a
negative test result does not have the disease (specificity).
In order to calculate specificity and specificity, we need to know a few
things, such as the incidence of the disease, and how our screening test
compares to the gold standard test. I guess here the disease is kernicterus and
despite attempts to figure it out, we do not know the incidence of kernicterus.
We also need to know that by screening our population, in our case, checking
their total serum bilirubin, we can prevent the disease in a meaningful point in
time, but kernicterus can occur without elevated levels of bilirubin. To
universally screen a population, early intervention should be beneficial in
preventing the disease from occurring. Again, treating high levels of bilirubin
might not prevent kernicterus. We just do not know enough about the disease, how
it is caused and what we need to do to prevent it well enough to subject every
baby and family to this testing.
One of the authors of the 2009 commentary said this:
-
“Guideline committees tend to be dominated by academics and subspecialists with special interest, expertise, and even emotional investment in the diseases for which they are producing guidelines. Most of us authors of the hyperbilirubinemia commentary are no exception. Although interest and expertise are invaluable, the career focus on a particular disease, with resulting close relationships with funders, patients, advocacy groups, industry, and each other, may lead to a narrow perspective in which heroic efforts at preventing or treating the target disease feel justified, even when a favorable balance of benefits over risks and costs is uncertain.” (Newman, T. B. (2009). Universal Bilirubin Screening, Guidelines, and Evidence. Pediatrics, 124(4), 1199-1202.)
I get being emotionally invested about the health and well-being of children or I would not have written this and I love that the obvious biases are acknowledged by the authors, but their passion, not their evidence, changed practice. I think the efforts and goals of breastfeeding mothers are truly undermined by their suggestion of universal screening for hyperbilirubinemia.
So, what are other experts saying? The United States Preventive Services Task Force (USPSTF), an independent body of experts that “conducts scientific evidence reviews of a broad range of clinical preventive health care services (such as screening, counseling, and preventive medications) and develops recommendations for primary care clinicians and health systems.
They say that:
there is adequate evidence that screening using risk factors and/or hour-specific bilirubin measurement can identify infants at risk of developing hyperbilirubinemia.
Not all children with chronic bilirubin encephalopathy (kernicterus) have a history of hyperbilirubinemia.
There is no known screening test that will reliably identify all infants who are
at risk of developing chronic bilirubin encephalopathy.
Early treatment can decrease the number of infants with elevated serum bilirubin levels.
However, the USPSTF found inadequate evidence that treating elevated bilirubin levels in term or near-term infants to prevent severe hyperbilirubinemia resulted in the prevention of chronic bilirubin encephalopathy.
They go on to describe harms of screening:
-
interference with breastfeeding
-
disruption of maternal-infant bonding
-
pain caused by heel stick or venipuncture infant weight loss
-
labeling of infants that have elevated bilirubin levels (the effect of labeling kids with jaundice has not been measured or quantified, but they acknowledge this may be important.)
-
Because of the lack of evidence, the potential harms and costs, the USPSTF concluded that “the evidence is insufficient to recommend screening infants for hyperbilirubinemia to prevent chronic bilirubin encephalopathy.”
So,
now what?
We have conflicting opinions on what to do.
I wrote all of this to get us thinking,
again, about numbers in context.
Current practice is based on expert opinion but there is potential bias in
expert opinion. Total serum bilirubin stinks as a screening tool, but the
concept of free bilirubin makes sense.
If the concept of free bilirubin makes sense, then our risk factors and
any screening tests should change to reflect those things that produce more free
bilirubin. Breastfeeding is normal, but we do not have any norms or protocols
based solely on exclusively breastfed infants for us to follow. Our screening
algorithms do not us to consider how well breastfeeding is going.
Nearly 25% of our babies are being supplemented in the hospital, at least
partially due to this screening and despite the encouragement of the AAP to not
interrupt breastfeeding when treating hyperbilirubinemia.
Most of us are in a
place that asks us to universally screen babies with some type of measurement of
bilirubin. We can help mothers and
babies by watching how we explain jaundice.
So many of the families in my own practice are scared about the level of
bilirubin because they were told of very scary, very unlikely, consequences of
high bilirubin. In healthy, term newborn
without hemolysis, we could explain that higher levels of bilirubin are expected
and then watch a feeding to make sure we are helping breastfeeding.
Telling mothers that we are checking to make sure their baby does not get
brain damage is just not supported by the evidence.
We can also help
mothers continue important practices like skin-to-skin and rooming- in by using
technology that facilitates these practices.
I love this suggestion from the
Indiana University School of Medicine:

(http://pediatrics.aappublications.org/content/early/2013/05/08/peds.2012-3479.abstract)
If you are in a place that simply will not do any of these practices, like watching a feeding, understanding the reliability of the screening test, considering rooming in and skin to skin while under phototherapy, or considering the USPSTF recommendations and someone recommends supplementation and we have no mother’s milk or donor milk with which to supplement making formula is the only course of action, a protein hydrolysate formula is the recommended choice. Protein hydrolysate formulas taste really awful and bring the bilirubin levels down faster.
If you have made it all the way through this, cool. The take home message: think about jaundice and what it means to that newborn and the family before we act.